In the hallowed halls of medicine, pathological diagnosis is revered as the “gold standard” for disease diagnosis. Its acuity rivals that of Sherlock Holmes, capable of discerning the truth behind complex symptoms to reveal the essence of disease. Each innovation in microscopic technology seems to infuse new vitality into the field of pathology, propelling it toward new heights.
01 Innovations in Pathological Diagnosis
◇ Historical Insights into Pathology
In 1858 at Berlin University, Rudolf Virchow—the founder of pathology—raised his rudimentary monocular microscope, ushering in a new era for the discipline. Little did he foresee that modern pathologists would one day examine diseases at the molecular level. As technology advanced, pathological observation underwent revolutionary transformations. From macroscopic structures visible to the naked eye, to the cellular world revealed by optical microscopes, to ultrastructures uncovered by electron microscopes, and finally to advanced techniques like immunohistochemistry and genetic testing at the molecular level—each breakthrough has granted pathologists new vistas. This centuries-long visual revolution has profoundly reshaped our understanding of disease, propelling pathological diagnosis from morphological description into a new era of precision medicine.

◇ Limitations of Gross Examination and Breakthroughs in Optical Microscopy
Before the advent of microscopic techniques, pathological diagnosis primarily relied on gross examination—where physicians conducted macroscopic observations of diseased tissues using the naked eye and simple tools. Holding scalpels, they carefully dissected diseased organs, meticulously examining tissue characteristics such as color, texture, size, morphology, and relationships with surrounding tissues. For instance, when observing tumors, macroscopic examination could preliminarily determine whether a tumor was solitary or multiple, assess the clarity of its borders, and identify the presence or absence of a capsule—information crucial for initial diagnosis and treatment planning. However, while macroscopic examination is intuitive and straightforward, its limitations are evident. It can only reveal the gross morphology of tissues and organs, failing to detect early lesions (such as microscopic cancer foci) or delve into subtle changes at the cellular and molecular levels.

In the 17th century, the invention of the microscope revolutionized pathology. Dutch scientist Antonie van Leeuwenhoek successfully constructed the world's first high-power microscope. This groundbreaking invention was further refined by Robert Hooke of the Royal Society of London, thereby expanding humanity's vision into the microscopic realm. Subsequently, in the 19th century, German pathologist Rudolf Virchow, hailed as the “Father of Pathology,” proposed the theory of “cellular pathology.” He firmly believed that “all diseases originate from cells,” meaning the essence of disease lies in alterations to cellular morphology and function. This theory undoubtedly propelled pathological diagnosis from mere macroscopic observation into microscopic exploration, thereby opening a new chapter in modern pathology.
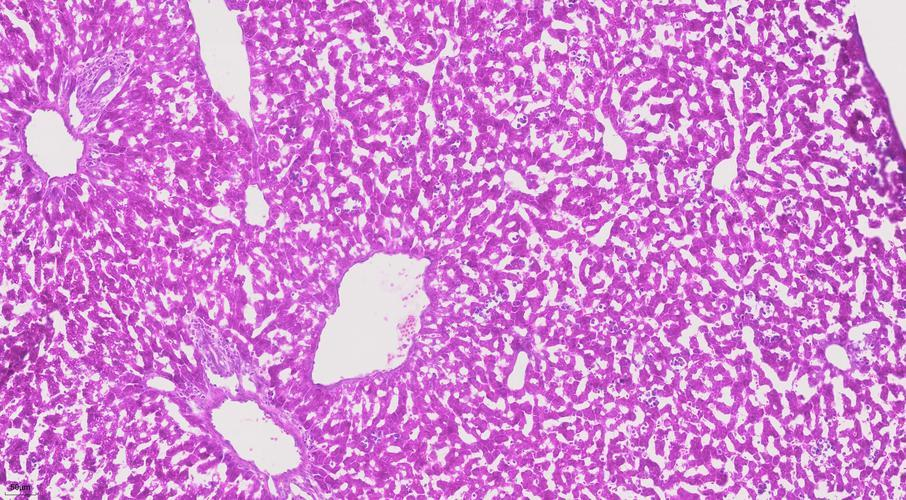
Following a series of processes—fixation, dehydration, and paraffin embedding—the patient's tissue is meticulously sectioned into 4-micrometer-thick slides. Subsequently, hematoxylin and eosin (H&E) staining is applied, rendering cell nuclei vivid blue while staining cytoplasm pink. Under the optical microscope, these stained cells revealed their morphological pathological alterations for the first time. Pathologists could visually observe the shape, size, arrangement, and distinctive features of cell nuclei.
◇ The Role of Electron Microscopy and Immunohistochemistry
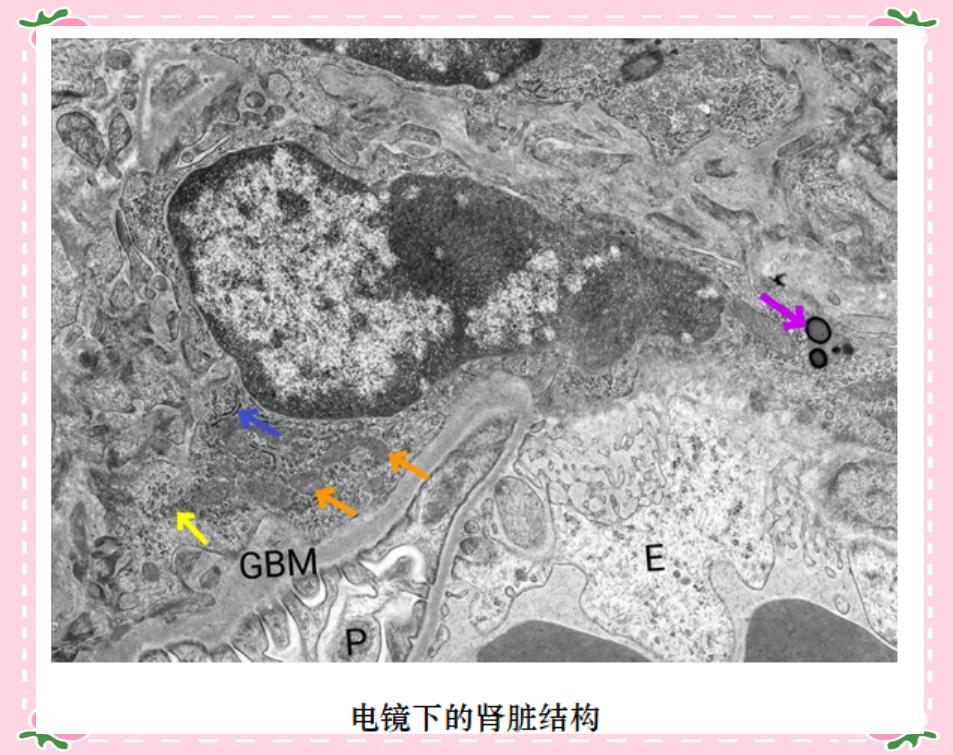
The advent of the electron microscope has vastly expanded human understanding of cellular ultrastructure. Abandoning the visible light imaging method of traditional optical microscopes, it employs an electron beam as its light source, thereby achieving exceptional resolution. With the electron microscope, scientists can meticulously observe intricate cellular structures such as organelles, cell membranes, and nuclei, and even reveal the detailed morphology of microorganisms like viruses and bacteria.
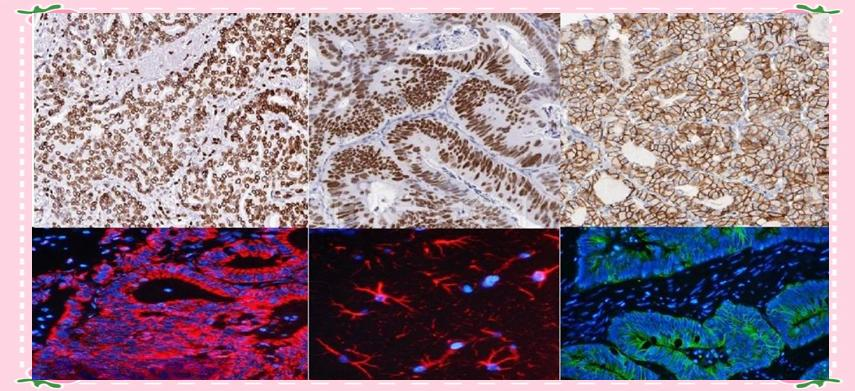
Immunohistochemistry, this remarkable technique that enables cells to “speak,” has significantly advanced pathological diagnosis. Relying on the specific binding between antigens and antibodies, it reveals the presence, location, and quantity of specific intracellular proteins by labeling antibodies that react with antigens within tissue cells and visualizing the antigen-antibody complexes using chromogens. This technique is akin to affixing a unique “identity tag” to each cell, empowering pathologists to more accurately identify cellular origins and characteristics.

◇ The Future of Molecular Pathology
With continuous advancements in life science technologies, molecular pathology has gradually emerged, expanding the scope of pathological diagnosis to the molecular level. This field encompasses multiple cutting-edge technologies, such as polymerase chain reaction (PCR), fluorescence in situ hybridization (FISH), and gene sequencing. These techniques empower pathologists to discern subtle alterations in cellular DNA and RNA molecules, thereby revealing the underlying molecular mechanisms governing disease progression and development.
In the field of tumor diagnosis and treatment, molecular pathology testing provides powerful support at the genetic level, helping pathologists make more precise diagnoses. Simultaneously, certain specific gene mutations are closely linked to the therapeutic efficacy of targeted anticancer drugs. For example, specific mutations in the EGFR gene in lung cancer often yield significant treatment outcomes when patients carrying these mutations receive corresponding targeted therapies. Moreover, molecular pathology techniques can be employed for early tumor screening. By detecting tumor-associated molecular markers in blood or bodily fluids, abnormalities can be identified before tumors manifest noticeable symptoms, thereby improving patient cure rates and survival outcomes.
Moreover, molecular pathology offers novel approaches to disease prevention and prognosis assessment. By studying disease-associated susceptibility genes, scientists gain deeper insights into genetic predispositions, enabling the development of personalized preventive measures for high-risk populations. Simultaneously, molecular-level test results can evaluate patient prognosis, allowing timely adjustments to treatment plans to ensure optimal therapeutic outcomes. Each technological advancement signifies more precise treatment for patients and marks another stride in humanity's fight against disease and the expansion of our diagnostic horizons.
In this visual revolution from organ to molecule, the “microscope” in the hands of pathologists is continually reshaping the boundaries of our understanding of disease.

Previous article:Advantages of Stains in HP Detection
Next article:Flaming Eyes: Pathologic Examination Makes Disease Diagnosis a “One-Time Deal”
Return to List-
Secured eight Class I medical device registration certificates, enhancing pathology diagnostic support capabilities.
2025-12-29 -
Special Staining in Renal Pathology Diagnosis: Applications
2025-12-29 -
Advantages of Stains in HP Detection
2025-12-29 -
Microscopic Technology Innovation: Reshaping the History and Future of Pathological Diagnosis
2025-12-15 -
Secured 8 Class I Medical Device Registration Certificates, Enhancing Pathology Diagnostic Support Capabilities
2025-12-09 -
Secured 10 Class I Medical Device Registration Certificates, Enhancing Pathology Diagnostic Support Capabilities
2025-11-27 -
The company has successfully obtained seven Class I medical device registration certificates, enhancing its capabilities in supporting pathological diagnosis.
2025-11-14 -
Flaming Eyes: Pathologic Examination Makes Disease Diagnosis a “One-Time Deal”
2025-09-09





 0752-2228195
0752-2228195